Introduction
Board of Directors
Objections Committee
Secretariat
ICHEIC
Applications
Payments
“Economic incapacity”
Introduction
The Stichting Individuele Verzekeringsaanspraken Sjoa (Sjoa Foundation For Individual Insurance Claims, hereinafter ‘the Sjoa Foundation’) originated from the agreement concluded by the Dutch Association of Insurers (DAI) and the Dutch Central Jewish Board (CJO) in November 1999.
The Sjoa Foundation was set up in order to assess and honour applications for payment of Jewish life insurance policies that had not been paid out after the Second World War. The objective is to find out whether people are entitled to a payment. A sum of NLG 20 million (€ 9 million) was reserved for this purpose. The Sjoa Foundation will handle applications submitted before 1 January 2010.
The Sjoa Foundation has been handling applications since 2000. At that time, a list of approximately 750 policyholders/insured persons of unclaimed policies was published on the Internet. Some 1,369 names were added to this list at the end of 2004.
The Sjoa Foundation secretariat researches traceable policies and reports the results to the Board of Directors, which then makes the decisions to allocate payouts to rightful claimants.
In addition, if policy details are unavailable, the Sjoa Foundation sends lists of names to all relevant Dutch life insurance companies associated with the DAI, which then go through their records, as far as they are still available, and report their findings to the Sjoa Foundation.
The first year was characterised by a great number of submitted applications, particularly after the first Internet list was published. At the time, the secretariat was not prepared for this volume of applications. In the subsequent years the secretariat was expanded and restructured. Staff increased six fold and clear procedures were introduced to deal with the applications.
Between 2001 and 2004 there was a consistently high number of applications, well over 2000 a year. It was only in 2004 that the number of applications started to drop to an average of 1,500 in the years 2004/2005. For the first time that year more applications were dealt with than were received. This was also because priority had initially been given to the most potentially successful, and therefore most labour-intensive applications.
The publication of new names on the Internet in December 2004 led to an increase in the number of applications, but no more new ICHEIC applications were submitted.
The number of new applications will probably drop drastically in the coming years.
As of 2001 the number of payouts rose sharply. In 2002 and 2003 this also led to a significant increase of the sums paid out. This dropped in 2004, due to the fact that many sums paid out in 2004 related to smaller inheritance shares of policies that had partially been paid out already.
The number of payouts rose again in 2005, but not to the level of 2002/2003.
Board of Directors
The Board of Directors comprises:
- Mr. M.R. Wijnholt, LLM., chairman
- Mr. E.J. Numann, LL.M., secretary
- Mr. J. de Ruiter, LL.M., treasurer
The Board of Directors met seven times in 2005 (2004: 8). During these Board Meetings 210 (2004: 303) reports relating to 426 (2003: 603) policies were among the matters discussed.
Objections Committee
The Objections Committee comprises:
- Mr. H.L.J. Roelvink, LL.M., chairman
- Mrs. A.S. van Leeuwen, LL.M.
- Mr. F.N. Meijer, LL.M.
- Mrs. M.A. Pach, LL.M.
Mr. W.Th.M. van der Velden is secretary of the Objections Committee and Mr. M.M.H. Timmermans, M.A. substitute secretary.
In 2005 seven (2004: 10) appeals were lodged with the Objections Committee of which one was settled with a negative ruling. Six appeals are still under consideration. Five current appeals were also settled, all with a negative ruling.
Secretariat
A secretariat was set up in 2000 to carry out the activities of the Sjoa Foundation.
The secretariat comprises six staff members:
- Mr. H.T.C.J. van der Well, project manager
- Mrs. J.T.H.M. Groenewegen, staff member
- Mr. J.M. Bas, researcher
- Mr.. D.R.W. Reijerse, LL.M., researcher
- Mr. J.A. Schaffers, researcher
- Mr. M.M.H. Timmermans, M.A., researcher
The number of staff increased in 2005 from 4,5 FTEs to 4.8 FTEs and averaged 4,7 FTEs over the whole year (2004: 5).
The costs of the Foundation are borne by the members of the DAI, who are historically involved in this matter.
ICHEIC
The International Commission on Holocaust Era Insurance Claims (ICHEIC), also referred to as the Eagleburger Committee after its chairman, was established in 1998. This Commission is made up of insurance regulators from the United States, representatives of Israeli and Jewish organisations, and insurance companies. DAI is a member of ICHEIC.
In 2001 the Sjoa Foundation and the ICHEIC reached agreement on how to handle applications submitted to the ICHEIC concerning Dutch insurance companies. The agreement was that our Foundation would handle all these claims and any payments would take place in accordance with the interest factors agreed to by the Dutch Association of Insurers and the Dutch Central Jewish Board.
The deadline for filing applications with the ICHEIC was 31 December 2003. Application forms already filled in could be handed in until the end of March 2004. Many took this opportunity and during 2004 almost 600 applications were received by us.
Registering these applications was very labour-intensive as the names and data provided were often wrong, misspelled and/or incomplete. In some cases the connection with the Netherlands was not clear. Each ICHEIC application can contain up to three different names (policyholder, insured and beneficiary).
Before these applications are entered in the regular registration, separate files are made and personal details are checked and supplemented where necessary.
At the end of 2004 not all ICHEIC applications had yet been entered in the regular registration. Approximately 200 applications had to be registered. This took place in the beginning of 2005.
Subsequently these applications were given priority and sent to the insurance companies for research. In 2005 all the names relating to ICHEIC applications were sent to the companies.
In 2005, 43 (2004: 599) ICHEIC applications were received. We compared our registration and that of ICHEIC, and it appeared that these 43 applications were not in our registration.

At the end of 2005 a total of 1,745 ICHEIC applications were received by the Sjoa Foundation, of which 95% were undocumented. Of these, 1,174 have been fully or partially settled.
In 2004 we sent 434 (2004: 291) letters containing decisions of the Board of Directors to the ICHEIC with the following results:
- 364 – no information found
- 48 – information about settled policies
- 20 – payments
- 2 – not taken into consideration
- 0 – withdrawals
CHEIC has undertaken to settle all applications by the end of 2005. In 2005, ICHEIC applications will therefore be given priority.
Applications
This year, 2,134 (2004: 882) applications were submitted, an average of 178 a month.
A total of 14,677 applications had been submitted by the end of 2005.

At the end of 2004 there was still a backlog with regard to entering ICHEIC applications in the regular administration. Some 200 ICHEIC applications still had to be registered. This registration took place in the beginning of 2005.
Making the assumption that 200 ICHEIC applications are equivalent to approximately 500 regular applications, it can be assumed that the number of applications for the year 2004 was approx. 1,400 and for 2005 approx. 1,600.
The applications can be divided into three categories:
- Applications that relate to a name on the Internet list with policies that have probably not been paid out (8%);
- Applications that mention an insurance company or a policy number (9%);
- Applications with no information about an insurance company (83%).
The applications received in 2005 can be broken down as follows:
- Category 1: 474 (22%) 2004: 88 (10%)
- Category 2: 212 (10%) 2004: 221 (25%)
- Category 3: 1,448 (68%) 2004: 573 (65%)
Due to the publication in December 2004 of 1,369 new names on our internet list, the number of applications in category 1 has increased considerably. This effect was particularly noticeable in the first half of 2005, when 87% of the applications in category I was received.
During 2005, applications in category 3 was given priority, especially the ICHEIC applications.
- In category 1, the percentage of settled applications in 2005 dropped from 91% to 62%.
- In category 2, the percentage of settled applications in 2005 was identical to that of 2004, namely 84%.
- In category 3, the percentage of settled applications in 2005 rose from 48% to 54%.

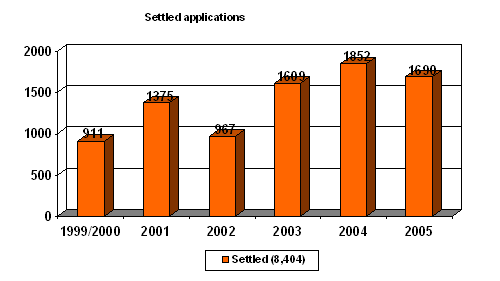
In 2005, 1,690 (2004: 1,852) applications were settled, bringing the total of settled applications to 8,404 (2004: 6,714), or 57% (2004: 54%) of the total.
In 2005, eight lists (2004: 9) containing 1,750 (2004: 1,089) names were sent to the insurance companies for investigation.
In comparison with 2004 bigger lists have been sent to the companies because of the finalization of the ICHEIC applications.
The applicants (in total 2,965) are mainly from the Netherlands, namely 57% (2004: 61%), but also 18% from Israel (2004: 17%) and 13 % from the United States (2004: 11%). These percentages are fairly stable.

Payments
In 2005, a total of 110 (2004: 102) policies were paid out to 916 (2004: 1,153) rightful claimants in the amount of € 660,305 (2004: € 358,175).
At the end of 2005 a total of 698 policies had been paid out to 4,168 rightful claimants.

The amounts of the payments per individual in 2005 were as follows:
| Payment amount | Number |
| Onder € 1.000,- | 768 |
| € 1.000,- tot € 5.000,- | 101 |
| € 5.000,- tot € 10.000,- | 14 |
| € 10.000,- tot € 20.000,- | 10 |
| € 20.000,- tot € 30.000,- | 3 |
| Boven € 30.000,- | 2 |
The largest payment was € 35,625; the average payment was € 720 (2004: € 310)
At the end of 2005 a total amount of € 3,267,643 has been paid.

The following pertains to the contribution of the current insurance companies in relation to the number of paid out policies and payments.
The seven main insurance companies and their most significant legal predecessors are:
AEGON
- Algemeene Friesche Levensverzekering-Maatschappij
- Eerste Nederlandsche Verzekering-Maatschappij op het leven, tegen invaliditeit en ongelukken
- De Olveh van 1879
- N.V. Levensverzekering-Maatschappij Nillmij van 1859
Delta Lloyd
- Hollandsche Sociëteit van Levensverzekeringen N.V.
- Amsterdamsche Maatschappij van Levensverzekering (Amstleven)
- Nationaal Spaarfonds
Fortis ASR
- Utrechtse Levensverzekering Maatschappij N.V
- Hollandsche Algemeene Verzekerings-Bank (HAV Bank)
- Gresham Life Assurance Society Ltd.
- Rotterdamsche Onderlinge Maatschappij van Levensverzekeringen
Generali
- De Nederlanden van 1870
Goudse
- De Oude Haagsche van 1836
- De Nederlandsche Spaarkas
Nationale-Nederlanden
- Nationale Levensverzekering-Bank
- De Nederlanden van 1845
- Rotterdamsche Verzekering Sociëteiten (RVS)
SNS Reaal
- De Centrale Arbeiders Verzekerings- en Depositobank (which incorporated the Nederlandsche Handelsreizigers Vereeniging N.V. NHRV)
- Zürich Leven
In relation to the number of policies paid out, the contribution of SNS Reaal was the largest (40%). This is because SNS Reaal was responsible for approx. 600 names on the internet list published in 2000. These names originated from their predecessor, De Centrale.
The contribution of Fortis ASR will probably increase in the future, because it is responsible for approx. 950 of the 1,369 new names put on the list in December 2004.

In relation to the amounts paid out, we see that Nationale-Nederlanden is responsible for the biggest share (51%).
De Centrale was an insurance company for workers, with mostly industrial insurances and small endowment insurances. Most of these policies are worth less than DFL. 500. The NHRV policies are valued at DFL. 1000.
Most of the new names on the internet list (about 850) came from the HAV Bank with an average insured sum of less than DFL. 200.

“Economic incapacity”
In several cases it appeared that the Council for Redress had refused to restore rights to policies after the war for the reason of “economic incapacity”. These involved life insurance policies for which during the war the payment of premiums had stopped and the policy was therefore cancelled or rendered paid-up.
Many of these cases were presented to the Council for Redress after the war. The Council specified two valid reasons for failing to pay premiums during the war. The first reason was in the case of actual circumstances beyond one’s control, that is, when policyholders had to go in hiding or were deported. In all other cases the reason was described as “economic incapacity”, meaning that policyholders were still free to choose whether or not to pay their insurance premiums.
According to the Sjoa Foundation’s regulations, these applications could not be processed, because a decision had already been passed by a court.
The following two examples illustrate the above:
- Nazi rules prohibited a Jewish doctor from treating non-Jewish patients, which meant that his practice basically folded. As a result, he could no longer afford to pay his insurance premiums. The Council described this situation as “economic incapacity”.
- In 1942 a Jewish man was arrested and imprisoned for several months. He was released at the end of the year but arrested again three or four days later. The Council’s view was that the man could have chosen to pay his insurance premiums during the few days he was free.
Nevertheless, the board deemed that in the light of today’s knowledge of the Jewish population’s predicament during the Second World War these rulings were unreasonable in the extreme. This opinion was endorsed by the Objections Committee, whose members were also assigned these cases.
After careful consideration the board made the following decision on 17 May 2005:
“Regarding those cases in which the Council for Redress refused to pay out on a policy based on its decision that, for Jewish citizens, the consequences of the financial measures taken did not constitute ‘actual circumstances beyond one’s control’, the board thinks that, in light of current standards, the unimpaired application of Article 3, paragraph c is unacceptable.
In recognition of the extent to which standards have changed, the board wishes to deal with these cases and will grant payment as compensation for the loss resulting from the Council’s decision. Given the foundation’s available resources, the interest due on the payment will be calculated using a factor limited to three.”
In 2005 the amount of € 52,230 was paid out on seven policies which had been judged on grounds of “economic incapacity”.
About seventy policies are involved here. We will process the applications we have registered and the names on the remaining policies will be added to the internet list.
The Hague, 17 May 2006
| mr. M.R. Wijnholt chairman |
mr. E.J. Numann secretary |
mr. J. de Ruiter treasurer |
